But that was before physics met the mechanical engineers behind Unity, a revolutionary device that achieves the medical equivalent of mixing water and oil.
Already in more than a dozen hospitals around the world, Unity is an 11-tonne giant that brings together the worlds of radiation therapy (RT) and high-field magnetic resonance imaging (MRI).
A decade ago, the mere idea of this seemed impossible. Proving it is possible gives doctors the ability to track cancer tumours as they move and to target them with never-before-seen precision. “It’s the most advanced piece of engineering technology I’ve ever seen,” says Dr Vivian Cosgrove, looking back at 30 years in radiotherapy. “It’s the most mind-boggling challenge.”
Cosgrove is the head of radiotherapy physics at Leeds Teaching Hospitals and a senior member of the Institute of Physics and Engineering in Medicine. He says he has no doubt the technology behind Unity will revolutionise the field.
Jennifer Anthony, a former radiographer who now works at Elekta, agrees.
“In theory it shouldn’t work,” she says. “The fact that engineering has overcome all the hurdles to allow us to see a tumour at the time of treatment and respond to it before we deliver radiation is game-changing.”
Defying physics
Radiotherapy, the act of blasting tumours with carefully controlled doses of radiation, is one of the reliable weapons oncologists have at their disposal. To administer the treatment, Unity’s linear accelerator uses microwaves to push electrons towards the speed of light. This happens inside a wave guide (a tube full of specially designed cavities) that’s 45cm long.
Once the electrons are moving at 97% the speed of light, they smash into an impenetrable sheet of tungsten. The collision forces the electrons to release energy in the form of light, or X-ray, which is then aimed and fired at tumours. The device revolves around a patient to spare as much healthy tissue as possible by changing its approach and firing radiation at the same target from different angles.
MRI scans, meanwhile, rely on powerful magnets to realign and map out protons inside a patient’s body. The patterns of shifting protons create radio waves, which in turn create the images doctors use to decide the best possible treatment. MRI scanners are incredibly sensitive and need absolute silence around them to ‘listen’ to the radio waves.
What MRIs don’t need is a particle accelerator speeding up electrons and smashing them into things. And what RT machines can’t stand is super-powerful magnets messing with their electrons. In short, the laws of physics dictate that RT machines and MRIs don’t make good neighbours, never mind room-mates.
Traditionally, doctors treating cancer with RT were forced to take MRI scans first, decide on a course of action and then do their best to target tumours. The trouble is, human bodies are like jelly inside and tumours move around constantly, even as patients breathe. This means collateral damage – healthy tissue being struck by radiation. It also means certain kinds of cancers, such as pancreatic, remain difficult if not impossible to treat with radiation.
Eyes wide open
Radiotherapy and MRI are not new technologies. They’ve been around for decades. Over time, both have evolved to become more precise. Radiation beams went from centimetres to millimetres and were shaped to match tumours with multi-leaf collimators (MLCs). MLCs are like camera shutters that use dozens of metal leaves to narrow and shape the beam, sparing as much healthy tissue as possible. Elekta’s Unity uses 160 leaves to create the right aperture.
Finding the tumours also became easier as imaging technology developed. Computed tomography scans were followed by MRI, which offered better soft-tissue definition. But doctors were still having to find the tumours in one room and treat them, later, in another, using a separate machine.
Imagine that radiation treatment is a surgeon’s knife and MRI is a pair of glasses. In the beginning, doctors were performing surgery with the naked eye and a blunt knife. MRI gave them glasses to see better, but they still had to take them off before performing surgery. MLC turned the knife into a razor-sharp scalpel, but the glasses problem remained. Now, with the arrival of a MR Linac machine, a doctor is able to keep the glasses on and use the sharpest possible scalpel to remove a moving tumour.
“It’s realtime imaging at the point of treatment,” explains Philip Arber, Elekta’s manager of mechanical systems. “This allows the treatment delivery to be optimised to match the tumour size and shape, which simply has to improve the clinical outcomes for our patients.”
Engineers to the rescue
So how did mechanical engineers manage to place a linear accelerator and an MRI scanner into the same machine? The answer has a lot to do with imagination, followed by years of design, testing and manufacturing. What emerged is a machine where the one device has absolutely no idea the other exists.
The exact details are a trade secret, but Unity’s linear accelerator sits inside a magnetic blind spot (or a ‘blind doughnut,’ since the Linac has to rotate around a patient). The MRI’s magnetic fields are distorted in a way that allows electrons to speed, crash and turn into photons without magnetic interference. The amazing part is that all this happens just centimetres from magnetic fields of 1.5 tesla.
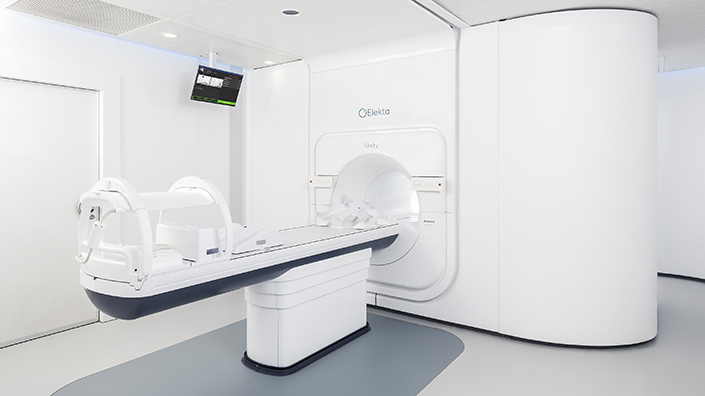
The Unity machine combines radiation therapy with high-field magnetic resonance imaging
At Elekta’s offices in Crawley, south of London, engineers working in development bunkers take great joy in demonstrating the magnetic power of the machine. A spanner is snatched from your hand like Thor’s hammer, flying into the tunnel. Try pushing a piece of (non-ferromagnetic) aluminium through the same tunnel and the air feels like thick liquid.
The electrons and microwaves inside the Linac machine need to be shielded from these magnetic fields but, once photons are released, they shoot towards the tumour as directed. Light is not affected by magnets.
Then comes the part where the MRI sensor needs radio-frequency (RF) silence. To achieve it, the scanner is placed inside a Faraday cage (also known as an RF box) that blocks out any noise. Traditionally, this would be a room or a bunker with a metal barrier running through the walls. With Unity, the barrier still runs through some of the walls, but it’s also built into the machine, curving with its lines, separating the MRI from the Linac.
Unity’s five-tonne gantry – the Stargate portal-looking part of the machine – is able to rotate at 6rpm, which may not seem like a dizzying speed, but, in the realm of radiotherapy, it means treatments can be administered faster and more cost-effectively, offsetting the price tag of a machine like Unity. The gantry is also able to spin continuously without having to back-track, thanks to innovative non-magnetic slip rings and cooling systems.
Smart solution
While building Unity, engineers had to solve “a million day-to-day challenges,” explains Duncan Bourne, one of Elekta’s principal mechanical engineers.
These ranged from choosing strong materials that could withstand radiation without distorting magnetic fields to making the machine less intimidating to patients. A wider entrance into the tunnel, for example, makes it feel less claustrophobic. It was all about finding the right balance between physics, mechanics and aesthetics, all under the pressure of a deadline.
The toughest part, says Bourne, is that all these problems had to be solved across time zones, language barriers and different CAD systems. Developing Unity took a consortium of companies and engineering teams across the globe, from London to Beijing. Virtual-reality software was used during engineering meetings to explore components, simulate operations and find faults quickly, without flushing weeks or months of work down the drain.
“We were able to fly around in virtual reality and find integration problems early on and correct them,” explains Bourne. “We used it as a core tool.”
Virtual reality proved useful in helping hospitals to design the bunkers – which include customised cranes, cooling systems and service platforms – into which Unity machines are installed.
“Another challenge was developing tonnes of high-tech equipment to be transported through a hospital and into a radiation bunker,” adds Arber. “Due to the high cost, there wasn’t a high number of prototype systems produced. System number two was installed in a hospital. Modules developed and manufactured in different countries needed to be integrated hassle-free.”
Looking to the future
In a machine with more than 30,000 components, smart engineering is everywhere. This includes the artificial rubies on each of the 160 leaves in the MLC. The rubies glow in ultraviolet light and allow operators to track their precise location and shape the radiation beam, without the need for more electronic sensors.
Clinical studies are under way to explore how MR Linac machines like Unity are transforming the world of radiotherapy and cancer treatment in general. Data is being collected and software is being developed to improve Unity’s precision and performance. Engineers are also hoping to soon see what they call ‘gating,’ which is a machine that repeatedly pauses the radiation blasts if the tumour moves outside the target. At that stage, a tumour will never leave the Linac’s crosshairs.
“As an engineer, you’re driven by the problem in front of you,” says Bourne. “But when you visit hospitals, and see the people waiting for treatment, that brings it home as to what this is all really about.”
Want the best engineering stories delivered straight to your inbox? The Professional Engineering newsletter gives you vital updates on the most cutting-edge engineering and exciting new job opportunities. To sign up, click here.
Content published by Professional Engineering does not necessarily represent the views of the Institution of Mechanical Engineers.