Especially as the recipient of the heart pump isn’t heading into space and space technology hasn’t been used in creating the device.
So what is the link? Problem solving, according to the engineer in question, Piyal Samara-Ratna, who works out of Leicester University’s Space Research Centre (SRC).
“Our key task at the SRC is to take the ideas that our scientists come up with and make them a reality. As most of these ideas are for things that have never been made before, and with space being such a challenging environment, it makes us very good at problem solving,” he explains.
As well as space projects, the SRC also applies its problem-solving skills to the development of products outside the space sector in what it refers to as space-enabled technologies. These don’t necessarily include space technology but have been designed following the same rigorous process. “I’ve mostly been involved in medical devices where a doctor comes up with an idea for a device but doesn’t have the means to take it forward,” he says.
This is how he came to design a novel heart pump. During an unrelated meeting in 2013, Dr David Adlam, associate professor and interventional cardiologist at Leicester University, discussed his idea with Samara-Ratna for a left ventricular assist device (LVAD) that could provide support for patients suffering with heart failure following a severe heart attack. Unlike current LVADs that require significant surgery for the pump system to be fitted inside the heart, his idea was to use a minimally invasive keyhole procedure for inserting a much smaller device between the heart and pericardium (the protective sac that surrounds the heart).
“Like oil in an engine, the pericardium holds fluid that keeps the heart working. Noticing that during a particular illness this sac fills with fluid pushing against the heart, his breakthrough question was, if fluid is able to compress the heart in a negative way, why can’t we use that in a positive way? So he wanted to show that the sac is strong enough to support a device that could compress the left ventricle, forcing blood to pump through the heart more powerfully,” says Samara-Ratna.
Funding boost
Samara-Ratna started out sketching ideas that he refined in CAD before moving onto creating some rough prototypes that were used in simple experiments with pig hearts. Having performed enough validation, Adlam approached the British Heart Foundation (BHF), which provided funding.
Now the development process could begin in earnest. Treating it as though it was a space programme, Samara-Ratna used problem-solving skills to work through what is required to build a successful prototype. In a space programme, it’s crucial to do this when considering that it costs £20,000 to send just one kilogram into space. If the mission fails, an extortionate amount of money would be wasted.
“When designing for space, the process is extremely important. You have to properly understand all the requirements and the risks in order to define your experiments as accurately as possible to prove that it works. You need to think about all the different failure modes rather than just jumping straight into a test and hoping to learn as you go,” says Samara-Ratna.
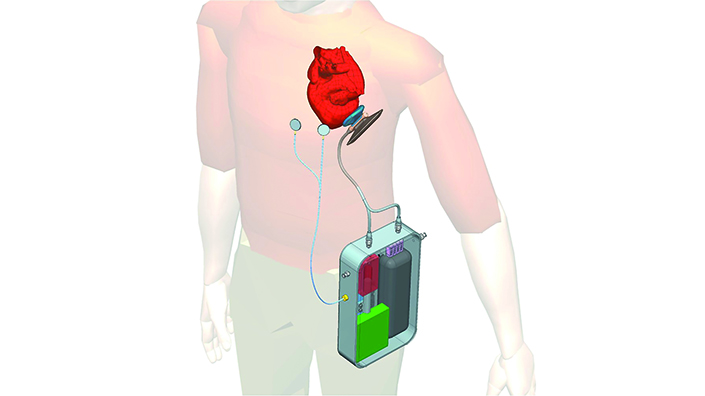
A concept image of the heart pump in action
While it’s difficult designing hardware for a harsh environment such as space, the human body is an equally harsh environment, and simulating it during the testing stages did prove challenging. “When testing space hardware, because it’s bits of metal, it often behaves reliably, repeatedly. Whereas we found testing in the medical environment to be much less reliable. We spent a lot of time performing both animal and cadaveric testing,” he says.
With the cadaveric studies, the doctors are even getting involved in the testing of the device. Using MRI scans (pictured) that have been imported into Siemens NX CAD software to reveal the inside of the body, they can study how the device is working.

“It shows exactly how the device is compressing the left ventricle and provides so much good information. The doctors pick up information that we just wouldn’t see at all. We then 3D print these using our in-house facilities and with these physical models we can see where it’s compressing a bit too much or not enough. It is really exciting,” says Samara-Ratna.
The technology, patented as PAL-VAD, is in the proof-of-concept phase. Following the regulatory approvals process, patient trials are due to start in two years. The hope is to also expand the device’s use beyond patients that need it as a short-term measure as the heart recovers from a heart attack, to those living with chronic heart failure and needing longer-term support.
According to the BHF, there are 920,000 people living with heart failure in the UK. “For these patients, their hearts are very poorly pumping blood around their bodies and if our technology can improve their heart output by 10 to 20% their quality of life will be improved,” he says.
Daily life could further be improved for these patients, because while the PAL-VAD, like existing LVADs, currently requires an external power supply, the hope is that with advances in battery technology it could become fully implantable in the future and recharged across the skin.
While that project is still a way off being commercialised, Samara-Ratna has in the meantime also been working on another space-enabled technology that has already been licensed to a manufacturer. It’s for a central venous cannula that offers an improvement to how doctors currently have to insert a needle into the jugular vein in a patient’s neck before they go into surgery.
“A doctor has to use an ultrasound probe to visualise the jugular vein before gaining access to it. The problem is that the procedure requires the doctor to use both hands to put the cannula device in, meaning that they can’t put the device in and hold the ultrasound probe at the same time.
“We were approached by Dr Atul Gaur, a consultant anaesthetist working in the University Hospitals of Leicester Trust, who had an idea for a one-handed cannula that would enable the doctor to gain access to the vessel at the same time as holding the ultrasound probe, allowing the doctor to clearly see how they can carry out the procedure and do so quickly and safely. This is a viable alternative to the established Seldinger technique which has been used for over 60 years, well before the use of ultrasound,” explains Samara-Ratna.
Before any prototyping was carried out, he spent time in surgical theatre observing how the procedure is currently being done. From there, ideas were sketched and modelled in CAD. Samara-Ratna was inspired to use small-diameter tubing that had been used in a Mars experiment. “Having already used this tubing for capillary flow action [the ability of a liquid to flow in narrow spaces] that gave me good confidence that it would work in the cannula in administering drugs into the body,” he says.
Prototypes of the cannula were produced and tested with clinicians in test models. Feedback helped to refine the design and, with a manufacturer onboard, attention had to be paid to ensure that it could be made as cheaply as possible using an automated assembly process. The team are now preparing for a trial to validate the device for commercial production.
Testing the heart pump
Software tools are enabling doctors to be involved in the testing of the heart pump within cadaveric studies. Called medical imaging, a cadaver is scanned using MRI technology. Essentially this involves taking sliced images of different sections in the body. For instance, tissue will be the same colour going all the way through the slices. So the software will work out that’s a 3D part.
These 3D MRI images are then uploaded into Siemens NX CAD software. This enables users to view not only the heart pump device working inside the body but also to view the heart, the lungs, the bronchioles and various passages. “We filled the heart with fluid that the MRI will pick up and we filled our device with liquid too. This enables us to observe the interaction between the device, heart and resulting augmentation of blood flow. When you look at the whole thing you get this amazing image of the dead person’s anatomy,” explains Piyal Samara-Ratna.
This isn’t just for use by the engineering team. Samara-Ratna has taught the doctors how to use Siemens NX and so they can view it themselves using their computers. The advantage of this is that as they are looking at it from a medical perspective they would pick up information that the engineers wouldn’t necessarily see.
These models are then 3D printed, allowing the team to physically assess how the device is compressing the heart. Feedback will then help to refine the design further.
Want the best engineering stories delivered straight to your inbox? The Professional Engineering newsletter gives you vital updates on the most cutting-edge engineering and exciting new job opportunities. To sign up, click here.
Content published by Professional Engineering does not necessarily represent the views of the Institution of Mechanical Engineers.