Introduction
An appropriate and up to date risk assessment should be the first step in determining appropriate COVID-19 mitigations within any workplace setting and ensuring that they are applied effectively.
In developing a risk assessment there are a number of considerations that can inform the approach taken:
1. Routes of transmission. Mitigation measures within a workplace need to consider all three routes of transmission: transmission at close range through inhaled aerosols and direct exposure to large droplets, transmission through the air at a distance (>2m) through inhalation, transmission via touching mucous membranes following contact with contaminated surfaces. The Figure 1 illustrates how different mitigations can potentially affect different routes of transmission
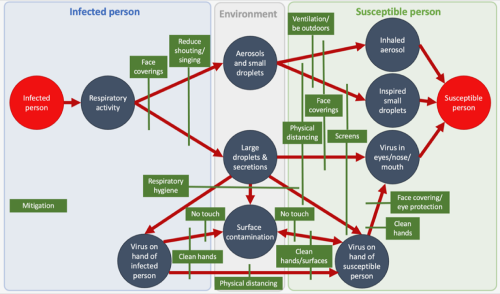
Figure 1. Visual demonstration of thermal camera output
(copyright Jay CCTV Solutions (JCS) Ltd)
2. Hierarchy of risk controls. This is a well-known risk assessment approach shown in Figure 2 below that recognises that some controls are likely to be more effective than others. This is usually because the more effective control is harder to circumvent by human behaviour rather than it is inherently less effective. For example enabling people to work from home is more effective than a strategy around hand and surface hygiene, because it prevents virus from entering the workplace in the first place. PPE sits at the bottom of the list as the measure of last resort; a mask may be very effective at preventing inhalation of virus from an engineering design perspective, but if it is not worn then it becomes useless and so to be effective requires appropriate training and processes to ensure compliance.

Figure 2: Hierarchy of risk controls highlighting engineering controls and with some examples of application to COVID-19
3. Actions outside vs inside the workplace: Preventing someone with the virus entering a workplace will be more effective at managing workplace transmission than using controls to limit the spread once it is present. This means that policies to enable employees and visitors to stay home if they are sick, to use COVID-19 tests effectively and to ensure people can isolate if they are a known contact of an infected case are as important to include in the risk assessment as planning practical steps such as distancing, ventilation and hygiene in a workplace. Strategies such as hybrid working from home and cohorting of workers into teams can be effective at reducing the extent of spread if there is a case within a workplace.
4. Consideration of all the activities and spaces: While it is tempting to focus on the main office space or factory floor, it is important to consider the full range of activities that happen and where they are located. Planning ways to reduce crowding in locker rooms or canteens can reduce the level of interaction between people. Ventilation of small spaces such as toliets, changing rooms and kitchen areas shouldn’t be overlooked. There is evidence for transmission in shared vehicles so mitigations such as good ventilation are important for activities where it is necessary to travel together.
5. Involvement of staff in the risk assessment: Mitigations are more likely to be applied well and understood if they are planning in collaboration with the people who use particular spaces. While organisations are likely to need overarching policies, local risk assessments need to consider particular spaces, activities and people who are involved. This includes identifying any employees, visitors or members of the public who may be particularly vulnerable.
6. Considering both environmental and human factors: The effectiveness of different measures will vary depending on the physical environment, the activities that are happening and the behavioural and socio-economic factors linked to those involved. Table 1 illustrates the relative risks associated with some of these factors
| |
Lowest risk of transmission |
Highest risk of transmission |
| Environmental factors |
|
|
| Proximity |
Always maintain >2m |
Regular close interaction < 1m |
| Duration |
A few minutes or less |
Several hours |
| Occupant density |
People spaced out, large space |
People closely packed, small space |
| Shared air |
Outdoors, well ventilated indoor |
Indoors with poor ventilation, recirc air |
| Environmental conditions |
Normal indoor temperatures, humidity |
Low temperature, low humidity |
| Viral emission |
Passive activity, face coverings |
Aerobic activity, singing, loud talking, no face coverings |
| Shared surfaces |
Rarely touch shared surfaces, good cleaning |
Regular touching shared surfaces, infrequent cleaning |
| Human factors |
|
|
| Contact frequency |
Case isolation, infrequent contact |
Daily, regular contact |
| Networked |
Contacts maintained within a small bubble |
Shared space with multiple strangers |
| Hygiene behaviours |
Regular hand hygiene, use of face coverings |
Poor hand hygiene, no face coverings |
| Occupational factors |
Small network, not public facing |
Care/health sector, public facing, long working hours |
| Socio-economic factors |
Work from home, able to isolate |
Poverty, crowded housing, inability to isolate for both space and financial reasons |
Resources
There are a number of resources that can support the risk assessment process and decisions on appropriate controls:
HSE provide significant guidance to workplaces including specific information on risk assessment https://www.hse.gov.uk/coronavirus/index.htm
SAGE have considered the balance of different activities and mitigations in a number of papers:
PHE Transmission Group, Factors contributing to risk of SARS-CoV2 transmission in various settings - 26 November 2020 https://www.gov.uk/government/publications/phe-factors-contributing-to-risk-of-sars-cov2-transmission-in-various-settings-26-november-2020
EMG/SPI-B/TG Mitigations to reduce transmission of the new variant SARS-CoV-2 virus - 22 December 2020 https://www.gov.uk/government/publications/emgspi-btweg-mitigations-to-reduce-transmission-of-the-new-variant-sars-cov-2-virus-22-december-2020
EMG, SPI-M and SPI-B: Considerations in implementing long-term ‘baseline’ NPIs, 22 April 2021 https://www.gov.uk/government/publications/emg-spi-m-and-spi-b-considerations-in-implementing-long-term-baseline-npis-22-april-2021